VROOM GROUP ∙ 2022
Aligning claims around assessors’ mental models
Web app
Internal tool
Background
In 2022, we were selling car rental policies through a well-known multinational insurance provider.
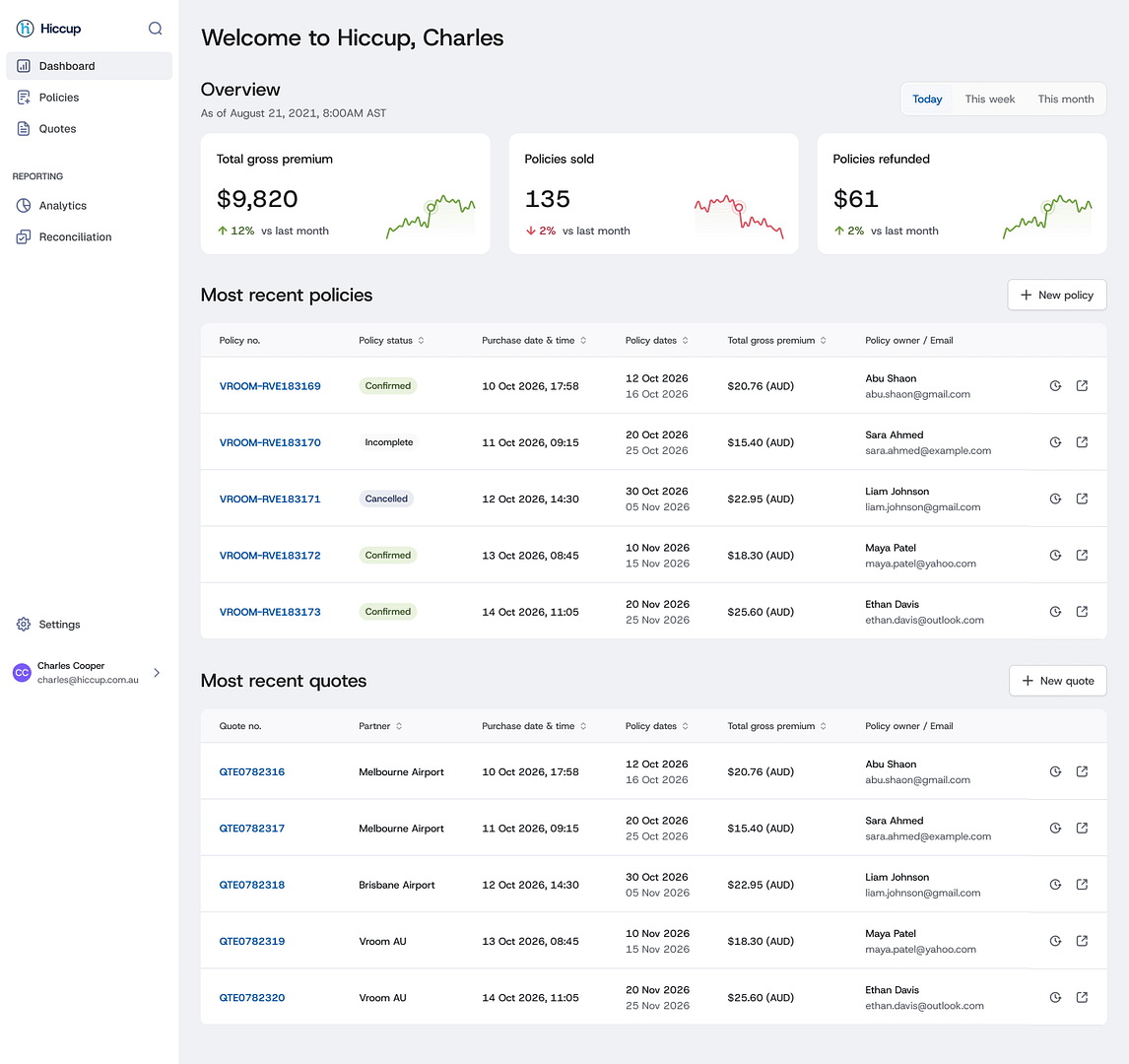
I had been the zero-to-one product designer who designed the cute, little internal tool to track our commissions.
But now that we were starting our own insurance company, we all had to learn how to handle our own claims.
My role
I took the lead on designing a dedicated claims workflow that would expand the capabilities of our current policy tracking platform.
Business needs
- We need a way to track, manage, and resolve claims internally
- Visibility into the status of every claim at any given time
Challanges
- There was no existing solution that was compliant with Australian rules and regulations and the specific needs of our underwriter
RESPONSIBILITIES /
Defined complex user flows to final UI execution and usability testing
Timeline & OUTPUT /
2 weeks to design an internal tool
TEAM /
PM, Front-end developer,
and Backend developer
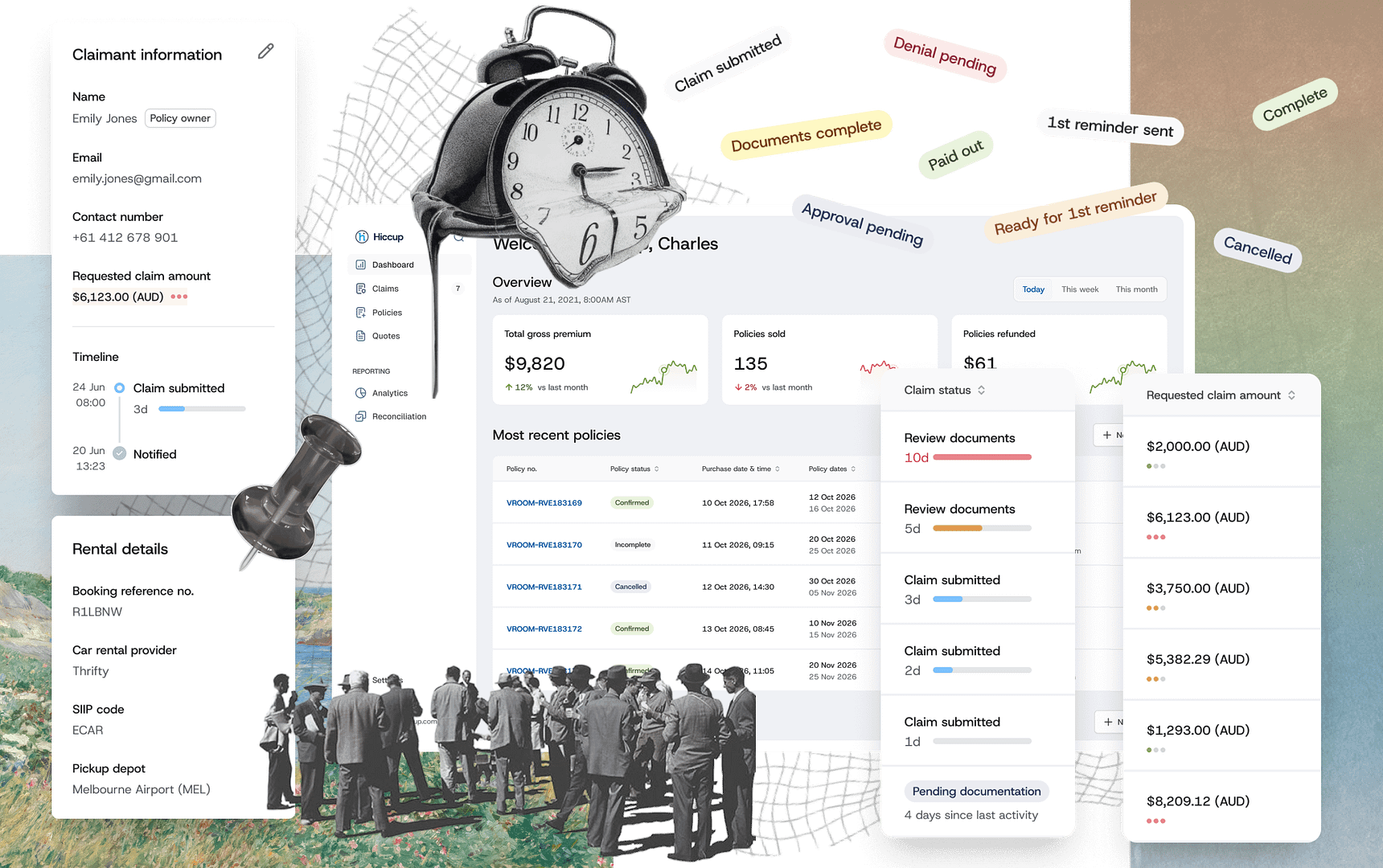
Welcome to claims
This was a unique situations where our internal claim handlers were developing their workflows alongside product!
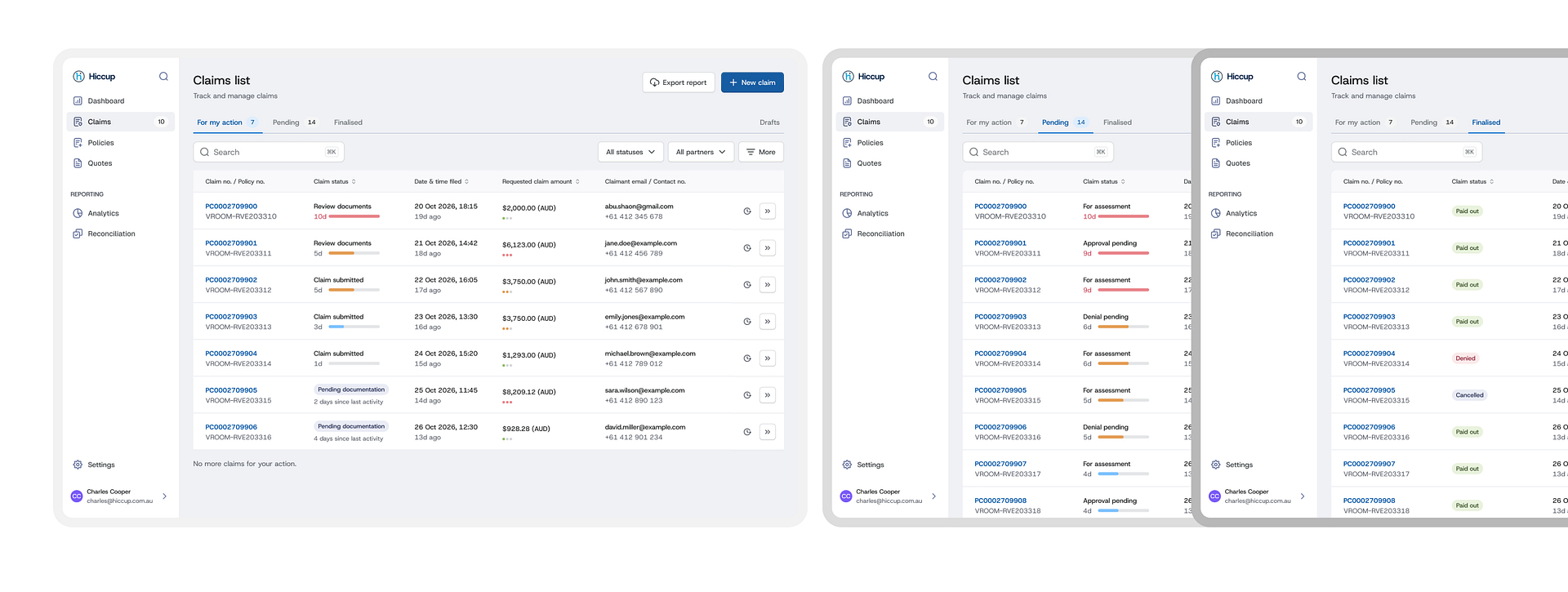
For my action
I introduced a "For my action" framework, designing personalized dashboards that dynamically surfaced tasks and statuses based on the unique responsibilities of each user type.
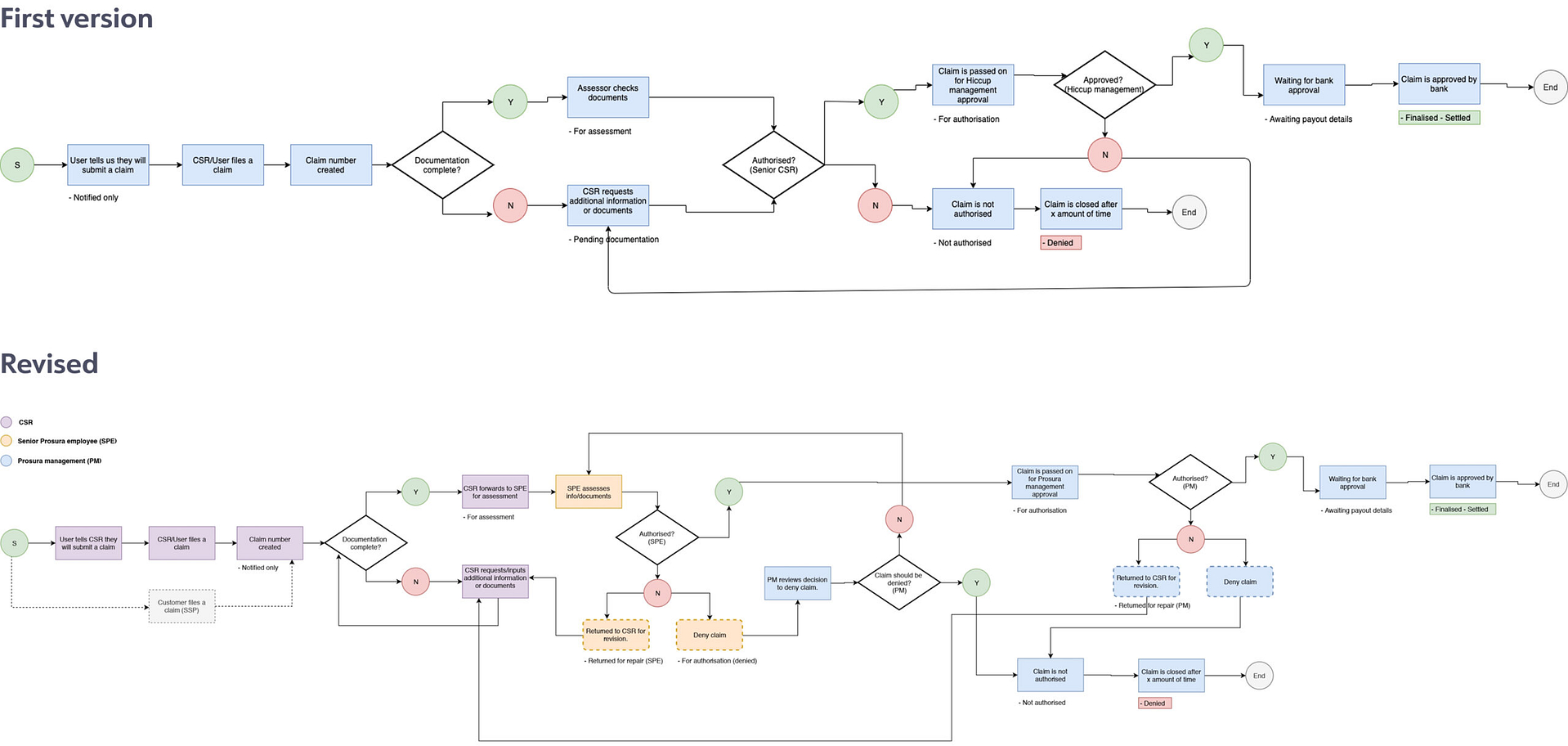
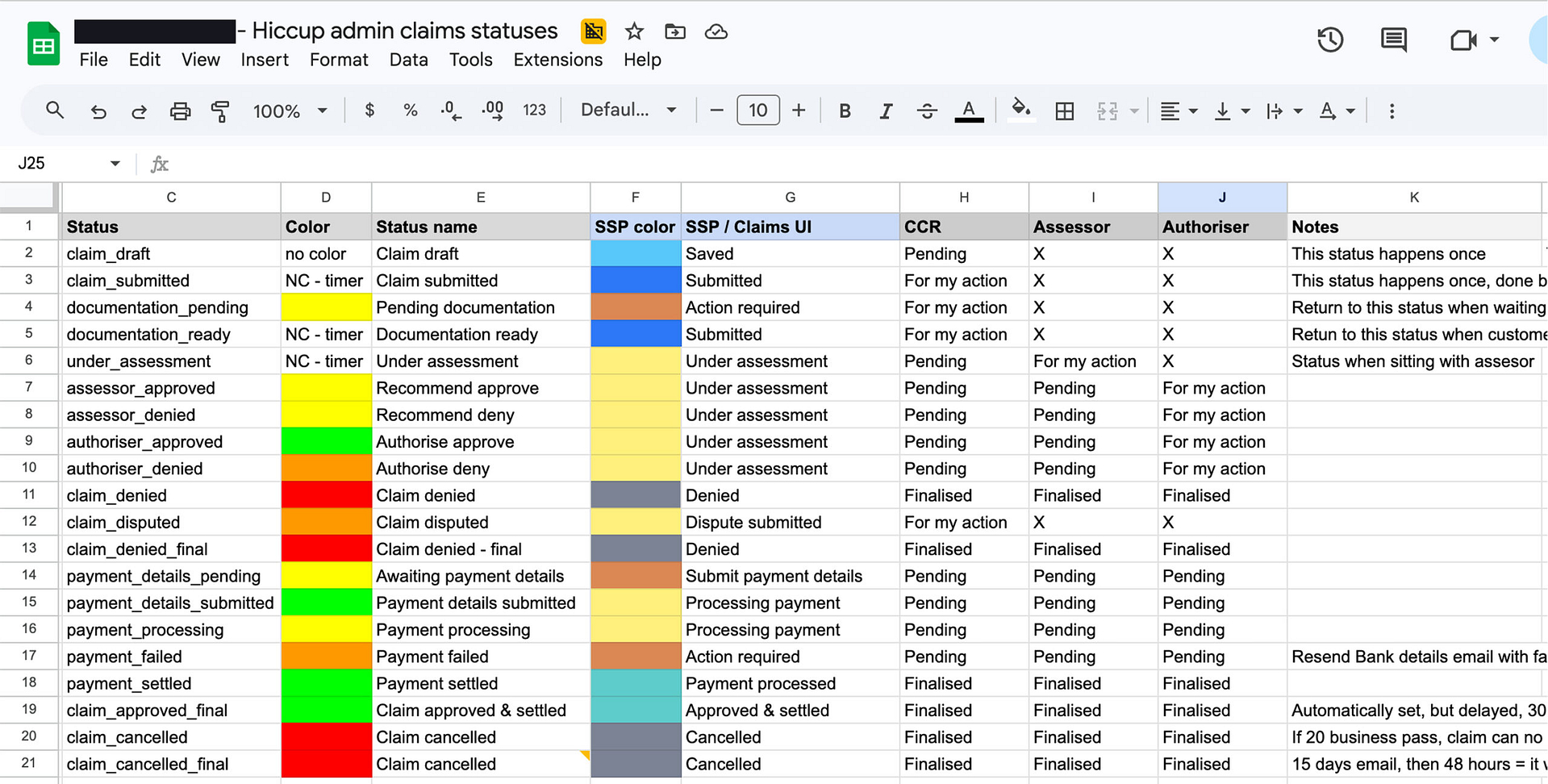
Status-mapping matrix
To ensure alignment between back-end system statuses, customer-facing labels, and internal operational views (Hiccup), I created a status matrix to map out the different layers. I collaborated closely with the dev team and operations in developing this "single source of truth."
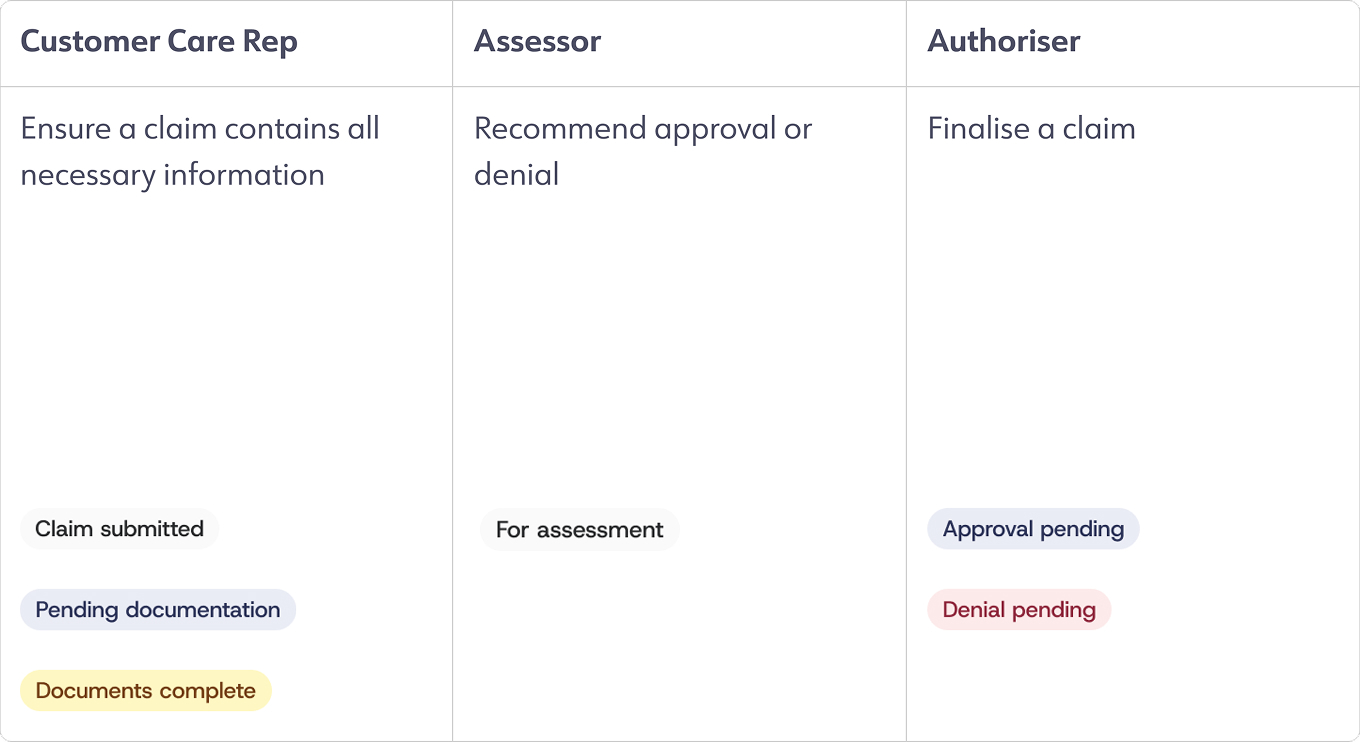
Three tabs, tri-tier logic
Each user type would have a tab For my action (active tasks sorted by SLA), Pending (claims currently owned by other user types), and Finalised (fully resolved claims). This way users could focus on their immediate priorities without losing the ability to search for or access any claim.
Impact & retrospective
01/
600+ claims processed annually
Despite competing operational priorities, a small team of 7 are able to process every claim through Hiccup.
02/
98.4% approved claims rate
This clarity has supported a 98.4% approval rate, ensuring that the vast majority of our customers experience a seamless path from filing to payout.
Key learnings
Involving users early: By mapping the key statuses with collaboration from our claims handlers, as well as a short round of usability testing, we avoided costly re-work and ensured the tool could serve the Ops team’s daily workflow.
Navigating compliance: Regulations are the ultimate design brief. When you treat restrictions as inputs, your designs are compliant by default.
💌OPEN MAILBOX
ALEXINE MARTINA ©
Made for alexinemartina.com by Alex